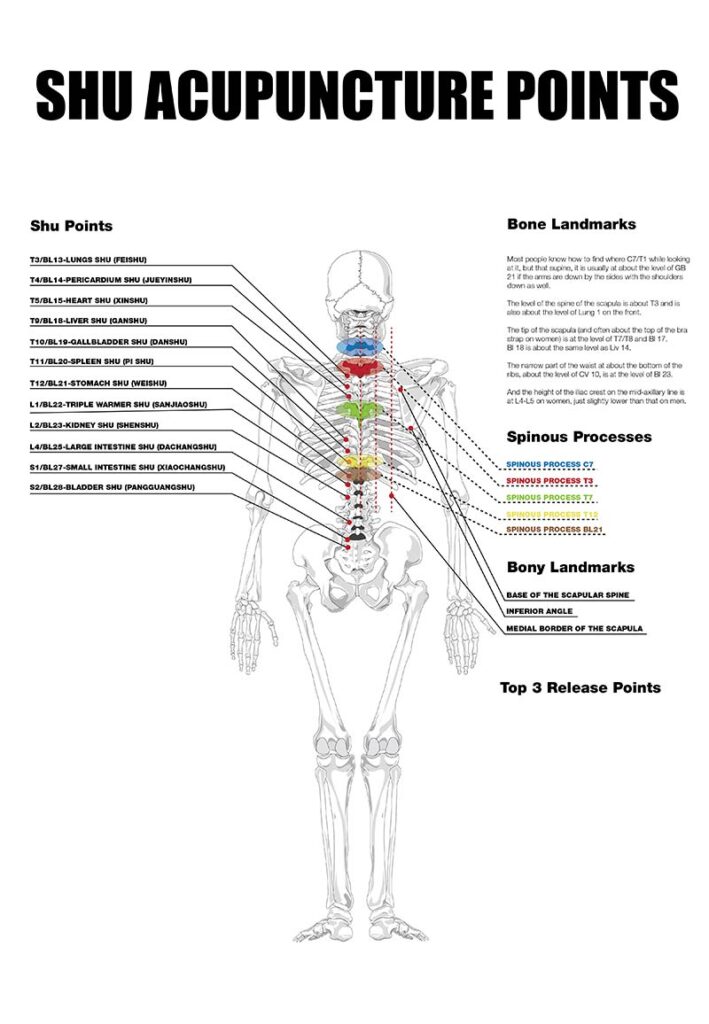
Q: OK, so tell me how you started developing the Back Shu Point System.
A: I think the first part of it came about with studying with Kiiko Matsumoto, where she would have all these reflex points, especially in the abdomen, and then she would touch a point and go, “Ah, it released. That means that this is the point we need to treat to rectify that,” whether it was the Adrenal Reflex Zone or something like that, or whatever. She has a lot of relationships. Or some of them are musculoskeletal, and using old [?] Lung 7 to 8, and like, “Ah. Yes, on you, that’s really good.”
And I started playing around with that more, realizing that, for me acupuncture was most exciting when I could find things in real-time. When it wasn’t so much of an intellectual exercise, “Oh, you have these symptoms; therefore, you must be liver qi stagnant, and we’ll do Liver 3 and 14 for liver qi stagnation.” Well, OK.
But then I got into going further, of realizing that you could test other things, as well. I think the first place that I noticed was people’s Bladder 23 being tight frequently. And like, god, well, maybe I could find something that would release that, that would open that area up. And I was like, well, it has to do with the kidneys, let’s try some kidney points. Yeah. But what was interesting was that it wasn’t the same on every person, nor was it the same every day.
It was almost like the chronotherapy, according to the hours or something—there were certain days where certain points were open, and I noticed that. Like some days, everybody Kidney 10 works on Bladder 23, or most everybody. Or other days, it’s more Kidney 7. So, I started playing with that, and then I went—people with other areas that were problematic, and it was like, well, where the hell am I? I’m at Bladder 18. Let’s try some liver points. And going like, “Oh, yeah.” And then, further going into taking someone’s pulse, and seeing that their liver pulse was both a little empty and a little tight, wiry, and it was like, well, what’s more important here? Tonifying or moving?
Well, their Bladder 18. I could figure out what was more important. Oh, Liver 8 releases it completely. Well, tonifying’s more important. Or oh, Liver 14 or 3 is the one that works. Oh, moving is more important for them today. It kind of helps refine my diagnosis.
And then, as I got further into it, I also realized that it could tell me the angle of the needling that was most effective. It could also tell me, have I stimulated enough, after putting the needle in, and it’s like, “It didn’t really release.” You stimulate it a little more, and it’s like, “Ah, there it is.” So, it’s kind of this real-time feedback loop. It’s like test, don’t guess.
Q: So, you don’t have to just do the same channel, like for Bladder 37, you could do Kidney channels. Sorry, 23. You’re sitting there, you’re palpating Kidney channels.
A: Yeah.
Q: Can you kind of do any point, or it tends to be channel paired, or channel-related–?
A: No, you can do anything. Like, for instance, let’s take the area of bai lu [?] or something, in the neck, or SI 15 area, that area that’s frequently tight on people. You know, Matt, one of his little nuggets is that for the levator scapula, the motor point for the flexor carpi ulnaris is often really affective. Well, so let’s say I’m on the insertion at the scapula, and boy, that’s tight. I can tell their levator’s nasty. Well, what I’ll do is I’ll put one finger on that, and then I’ll use the other fingers on the other hand on the motor point of the flexor carpi ulnaris, and if it melts right away, it’s like, yeah, that’s the point.
And it’s not on the same channel, per se, but I also know that other points are useful, like sometimes, it’s the small intestine point, because it kind of goes right through that area, the small intestine channel. Or from old Chinese style, Lung 7 is the master point for the whole neck area. So, a lot of times, I’ll just feel that, and I’ll palpate two or three points in close succession and go, “Oh, that’s it.” And it’s like, “Lung 7 feels a little better, but not all the way better,” so then I’ll traction it towards 8, and then it’s like, “Oh, that’s it. I’ve got to angle it that way for the best affect.” Does that make sense?
Q: So, there’s not necessarily specific needling techniques, again, it’s just testing to figure out what technique would work.
A: If you have the time, or you’re not getting a clear answer. And sometimes it’s a paired meridian, occasionally. Or sometimes you’ll have bleed-through. It’s like, oh, 18, OK, I’ll test all the liver points—well, nothing really—well, let me check Gallbladder, and it’s like, oh, it’s a gallbladder point. Because I thought it was 18 but it was really 19—whether I was feeling in the exact right spot, or that the gallbladder was affecting the liver—that sometimes happens, too.
Q: I’m trying to get a treatment flow in my head. Do you palpate and then do the pulse, tongue, and talk to them, and you kind of have an idea, and then test the Shus? Or do you test all the Shus, and go, “Oh, that seems super tight,” and then ask some questions about that? Or how does that—because definitely, you can use it to help direct your diagnostics, but when does that testing flow happen, like in the—naturally, when you’re treating someone, how does that flow work?
A: Well, it’s changed over the years. It used to be pulse, tongue, all that stuff, and then maybe abdominal palpation and then the Shu points, and it’s often that way in new patients—that’s often the flow in new patients. But for repeat customers, where I know kind of their general, underlying situation, I will often omit the tongue and sometimes the pulse and go right to their tummy and there back. As I’ve gotten more competence in it, the back has gotten more like my go-to. Like, especially for balancing.
For instance, I’ve got a big musculoskeletal component that I need to do, but they’re a little—they’re pretty tight, or they’re pretty weak, I may start with a short course of points that I garner from doing my Shu point diagnosis. And then, I’ll go—and that will relax them, it will balance them, you’ll get them kind of organized for—OK, I want to really fasciculate that muscle, and I want to rebalance this, and maybe use some electro. If I went right to it on a lot of people, it’s a little jarring, coming from their daily life. Plus, just balancing them, it makes the musculoskeletal stuff work and stay better.
So, I would say that it’s taken more of a primary role in a lot of my work with people—that and manual muscle testing, for a lot of my more sports-acupuncture-oriented things. If they’re there for digestive concerns, it’s much more about tongue and pulse, or if they’ve got menstrual issues—kind of the more internal medicine, TCM paradigm probably takes more primacy.
But I’ll add in the TCM. It’s like, oh right, you said you have stagnant blood, it seems from your pattern, your tongue and everything. Well, what points are most effective for you? And then you kind of glance, you go through, and oh, Bladder 20’s tight. Well, what point? Is it Spleen 4, which moves? Spleen 8? Spleen 10? So, I’ll test those points. Oh, it’s Spleen 10. That’s really good for gynecology, that makes sense. Or 18’s really tight. Well, it should be 3 or 4 or 5, they both move a lot. We want to move the blood—oh, yeah, it’s 3. That makes sense. Or their digestive concerns. Oh, yeah Liver 13, yeah, it’s the move point for the spleen, that makes sense.
So, it will inform my internal medical treatment with acupuncture, but I’ll probably put that more toward the back seat, whereas with other conditions it’s more in the front seat. But it’s usually there in all my treatments.
Q: Which treatments is more in the front seat versus ones that are in the backseat, I don’t know if I got that?
A: Like, if I know that you’re coming for your shoulder condition, you know, the first time, I’ll check your tongue and pulse, and all of that. But I’m more—for that condition, I’m more interested in your manual muscle testing. And then I’ll then, for balancing you, I’ll do a quick scan of your Shu points. So, that’s more front seat.
Q: You would kind of use the Shu points before you would do the trigger points to kind of get them relaxed—
A: Oftentimes. Yeah, just to get them balanced and get things organized for the next piece, because if they’re already coming in kind of imbalanced, and you go right to an area that’s already a little jacked up, so to speak, neurologically, for a lot of people, that’s intense. But if you ground them, or you tonify them, or let’s say they’re really liver qi stagnant, and you don’t address that first. Every point, they get a similar, it’s like, “Ah! Ooh! Ee!” It makes it less comfortable for them, and it makes it much less smooth for me, in my flow. It’s more like, “OK, how are you doing?” You have to slow way down—so by balancing some of that stuff up first, then you can go into it, and you get much less reactivity that can be difficult for them and sometimes you.
Q: Yeah. So, I’ll palpate the Shus, and sometimes I’ll find multiple tight spots.
A: That’s usual.
Q: Or I’ll find a tight spot—OK, so my question is, what happens if I find multiple tight spots? Or what happens if I find a tight spot that’s not painful to the patient, or I find a tight spot that is painful to the patient? Is it more about what the patient feels, or more about what I feel, or kind of a combination of both?
A: Combination of both, but primary is what I feel, what you feel. A really common example is, I’m scanning the medial scapular area, it’s like, “Oh my god 42 is like crazy,” and they go, “Ow, god!” “Yeah, you didn’t mention anything about your shoulder.” “Oh, that’s always there. It’s been since I can’t remember when, and it’s nasty.” And I go, “OK.” So then, I’ll palpate some Lung points or some pericardium points, in case I was one off, and it will be like—boom, it melts under my fingers. So, I’ll put that in, and it’s like, you can just see them kind of go, “Ahh.”
A common pattern would be maybe one from the upper Jao [?], you know that, like 42, and maybe one from the middle Jao, like liver, and maybe something down low. Like you’ll find three, or two. And then I’ll just pop those in. And sometimes, right after I pop them, I can go right into something else, but I always feel like it’s good to balance them.
And whereas I used to, like, “OK, what’s going to be good to balance them? Maybe four gates—” this is more tailored to them in the moment. And they may have different things. Some people come back with the same ones, repeatedly. Other times, you treat it and it’s gone. Like, “OK, that was easy.”
Q: And it’s really a—because that’s the other thing is I’m like, “Well, did it melt?” But it should be pretty pronounced if you get it—or what if it’s like kind of—you know, because I’m new, it feels slightly better, and I ask them how they feel, and they go, “Oh, it’s slightly better.”
A: They often—a lot of people can’t tell. They don’t live in their bodies enough—I mean, some people are really sensitive to what’s going on, and they really get it. But some people don’t really understand what’s going on or feel it. It’s more what you feel. And if it’s the best point you did, go back and tickle it as you’re stimulating the other point, because that opens up, again, a linkage. Like, “Hey, I’m talking to you at this point.”
Like I might be at Bladder 18 and with Liver 8, and it’s like 50% better, but I’ll go, “Let me angle it a little differently,” and it will be like, “that was it.” Or maybe it just needs a little extra lift and thrust or twirl or something, and then it will go another 20%. It’s not that it melts 100%, but that there’s a change, in real time. Because the point will continue to work after you pull it out, but you want to have a significant shift.
Q: OK, so if there’s multiple ones that you feel—
A: Yeah, I might pop in Lung 9, Liver 8, and Kidney 3, or something. Or Stomach 36 and Pericardium 6 or something, you know.
Q: Would one point—so, say I have like a Neck, Bladder 13, and then the kidneys, Bladder 23, and they’re both tight. Do you find that one point will relax both of them, or do you tend to find that you have to find two different points for both of them?
A: Usually I find two different—sometimes if they’re related…
Q:And then do you feel like you have to treat all of the points, or just what relates to the symptoms, like if they’re going, “Oh, I have…”?
A: No, I understand. One, it depends on the individual. Like a sensitive person who, in the back of my mind, I’m thinking, “If I get 10 needles in them total, that’s going to be a good day,” because, especially someone new, they’re like, “Who the hell is this guy? What is acupuncture? I’m a little weirded out by this whole thing.” I’ll winnow it down, like, “Oh, you have digestive concerns, and Spleen 6 is releasing Bladder 20 and 21?” I’ll do that one, and I’ll let their upper Jao, their Bladder 13, go today. But I’ve noted it. I’ll usually make a note of which Shu points and what points release them, off to the side.
Q: OK, so you do have like a couple Shu points and like common release ones.
A: Sure, yeah. That’ll be in my June class.
Q: Oh, cool. And they tend to be paired, like channel pairs?
A: Tend to be, not always. Like sometimes Spleen 6 is the best point for the liver. But the liver courses through there. Or the sacrum. Bladder 27 isn’t often small intestine points.
Q: When’s your June class?
A: It’s like Saturday the 2nd or something. It’s half a day, it’s the OCOM Alumni free event.
Q: Oh, OK.
A: Yeah, I’m doing like 1:00 to 5:00 or something. And they said, “Well, what should you do?” And I said, “I don’t know, people ask me about this.” And they said, “Oh, yeah, do that.” So, I’m going to try to impart a lot there.
Q: That will be good.
A: Is this helping?
Q: Yeah. Oh. I treat most people laying face-down. And you treat most people laying face-up.
A: I do. Or at least I’ll start there, and then I’ll flip them over.
Q: Yeah. I imagine it would be the same face-down, except it’s harder to kind of get to some points?
A: What are you asking about, about the Shu Point diagnosis?
Q: The Shu Point diagnosis.
A: I find that it’s easier to access all the points that you’re wanting to addition, so to speak, with them supine, with them face-up. The only things you can’t really reach are the back Shu, and you’re using them, anyway, because you’re maybe trying—everything else is pretty accessible when they’re supine, other than the ones you’re actually lying on. Secondly, when they’re lying on them, for some reason, I get more of a neutral feel from the areas that aren’t involved.
Q: When you’re lying on them, you’re getting more of a neutral feel for the areas that aren’t involved.
A: Like the figure ground, like who’s important, sticks out better than if I’m going like this. And it’s probably just because I’m used to it. I’m sure that one could cultivate the sensitivity in another position. It’s just more convenient like, I’ll find something in their abdomen, I want to see what releases that. Or I’ll find something in their neck. You can reach their whole neck this way. Or something in their sacrum. OK, what point releases that? Or all the Shu points, what point releases that? So, I have more availability to get to—sometimes the liver, it’s Liver 14 or 13. I think it’s just convenience, plus, a lot of times, I find, both with doing the treatment, I want to watch their face. I want to watch their color change. I want to watch their eyes go like this. I want that feedback, because I know that, “Oh, they’re feeling that.” Or, “Oh, there’s the stimulation.” Or, “Whoa, I need to slow down, their color just shifted, and it got a little pale or got a little green. OK, we need to take a break. You could get shocky.” Or they get a little yellow. That’s a good sign.
Q: Yellow’s a good sign?
A: It can be, yeah. Real light, just a teeny shift. Or they’re getting red, or you watch the musculature in their face just kind of melts, it’s like, OK, good. They’re going to be much better when I want to dig into their hip with a three-inch needle. They’re chilled-out.
Q: So, then would you then half-way rotate someone over, and do the motor points—like how does that work? Would you flip someone over if you wanted to do like SI 12 or something?
A: Yeah. I find I get anywhere from 60 to 80% of what I want to do—or sometimes 100% with them supine. Because the only things you can’t reach are bladder points, and like SI 15 or 12, or something. Some of that stuff. And then I’ll flip them over. Like for instance, let’s take a shoulder—a real common one we were talking about, like with you—the big piece of work is your sub-scap. That’s what I really want to focus on, because that is going to turn on your supraspinatus. Now, might I flip you over at the end and just hit the supraspinatus motor point for a few minutes? Sure. Or, you know, the levator insertion point if the levator’s involved, yeah. And maybe a distal point to balance Bladder 60, or something.
So, yeah, a lot of my treatments are more weighted toward a supine treatment, just because I can watch their face, I can reach most of the points. But sometimes it’s not. I mean, like—
Q: I feel like that answers my question. Is it always both sides, or can it be just one side?
A: Oh, that has that pattern?
Q: That has the tension, like—
A: Yeah, mostly it’s bilateral, but sometimes it’s not. Especially it’s—oh, let’s say it’s a computer program, who’s constantly—they have mouse-shoulder. They’re going to have it more on their mouse side.
Q: Yeah, so for a beginner, for someone who’s just trying to start out, most of the time it would be a bilateral.
A: Yeah, especially if you’re looking at more internal medical stuff or balancing.
Q: And are you doing—can it be more of an internal bladder point, could it be an external bladder point, or is it just the tight of the erector spinae? Could it be anywhere along there, or is it more specifically—
A: It’s usually—huh, that’s a really good question, actually. It’s usually the inner bladder line. But in the scapular region, it’s often the outer bladder line. But they’ll have the same correspondence. Like Bladder 43, think pericardium point. But the lower—and sometimes it’s true for some of the lower points, like let’s say Bladder 52. That’s another one. Some people call it an adrenal-oriented point, or anyway, it’s related to the kidneys. Well, it’ll be a kidney point, nine times out of ten that will release it.
Q: So, when you find a Shu point that’s active, and you’re testing points to see what relaxes it, and—are you using like a five element, are you using traditional Chinese medicine points, are you using—what system of thoughts would pull up those points?
A: Usually kind of TCM or associated meridian is the first level.
Q: It’s not like [indiscernible] point on the thumb, or—
A: It could be—
Q: In general, you’re not—with TCM, it’s always case-specific, but I’m just saying, in general.
A: Yeah, but like the example I gave for the levator, how sometimes it’s like, I know from my work with Matt, the flexor carpi ulnaris will release that 15 area—that’s not particularly TCM. Or the sacrum is a meridian perspective. Sometimes it’s a meridian perspective rather than TCM, per se.
Q: And in the supine position—I mean, I guess the Mu [?] points don’t really have a muscle [indiscernible]. Do you test the Mu points?
A: Do I palpate them?
Q: Is that—
A: I sometimes do, but I don’t always necessarily—it’s more the exception than the rule. Like for instance, somebody’s really tight here at CV [?] 14-15, well, that’s kind of fire-related, and some people say the heart. So, I may just go, “Oh, let’s check Heart 7, 6, 5, 4, 3—oh, 3, oh yeah, it releases that. Oh, cool.” But it’s less common. I use the Shu points for my Mu points.
Q: Oh, OK.
A: Because after years of palpating the Mu points, I didn’t find I garnered any really clinically useful information very often. Like for instance, with gallbladder problems, palpating Gallbladder 25, it’s usually like, well, maybe, but there are other points that are way more responsive, like the Gallbladder Reflex point on the ribs, or SI 11 on the right, or there’s other points that are crystal clear, and that I get more clear information that I can test against what point releases it, rather than Gallbladder 25. The number of times I’ve found anything of interest at Gallbladder 25 are pretty small, but the number of times I’ve found something here at the ribs, or at the shoulder, are a lot.
And maybe it’s just that I don’t—when you—I haven’t used them enough to garner that kind of fine discernment. Like some people, it’s like—you know, people who take the pulse and go, “Your aortic valve has a problem,” or, “You have this—this happened when you were a kid.” People can tell all sorts of stuff if you study stuff long enough.
Q: So, the flow of your treatment. The patient comes in—new patient. You would do a traditional test.
A: Intake, you know.
Q: Say they’re coming in for internal issues. Gynecological issues, you would do a typical kind of intake—
A: Yeah and really drill down on what’s their menstrual flow like, and is it painful, and you know, all the questions, much more expanded menstrual intake than I would with just somebody else.
Q: And then you would do tongue and pulse—
A: Correct.
Q: And then in your head, you were thinking, “OK, I have a traditional Chinese medicine diagnosis,”—
A: Mhm.
Q: And then you start testing. Is that kind of—so then you would have them lie down and start testing the Shu?
A: Yeah, and/or the abdomen. For instance, with someone with a gynecological case, the abdomen because really important. Like, “How’s the Chung-Mai [?] feel in the abdomen? Oh, wow, it’s like two chop sticks in there. Well, that tells me something. That kind of goes along with their problem.” And well, with that, let’s just check, oh, Bladder—and this will often happen. “Upper Shu, oh Bladder 43 is really tight. Oh, I bet I know what point’s going to release that. Pericardium 6 because it’s already part of the Chung-Mai treatment,” and most of the time, that’s true. And I’ll go down, and it’s like, “Well, probably, we’re going to find something in the liver, just guessing.” And it’s like, oh, hell yes.
And it’s like, for grins, I might try Spleen 4 or 6, but it will often be like Liver 3 or Liver 14 will be a really important point for that person, to add into the mix. And I won’t necessarily do all those points, but it will sort of be like, “Oh, OK, so that’s important,” and already, you think liver, but it’s sort of like, “OK, well, is 3 the most important point today? It might work, but what point might be—maybe there’s another point I could use with it.” Like if I have 14, I may do 3 and 14. But I wouldn’t leave 14 out, because I know that her body has a big release reaction to that, and things are being held tightly. And I would do the Chung-Mai to open up the Chung-Mai.
Q: So, you get that all balanced out. And then, do you let them sit? Do—
A: You mean with the needles in?
Q: Yeah.
A: Yeah, sure.
Q: OK, and then you come back, and then do you layer anything else on top of that?
A: Depends. You said like their first treatment? Probably not. Especially if they’re not like, “Oh, yeah, I saw an acupuncturist for 20 years in San Francisco,” they’re old hands. And again, I’m watching their face. Are they like puddles? It’s like, “Oh, yeah, you’re done. You’re cooked. Any more and you won’t be able to drive home.” Or, “Yeah, I feel better.” And I’ll just feel around and go—it’s one of those clinical judgement pieces. Or the sensitive person who’s just coming in for their first one. I might just do the Chung-Mai and then let them sit. Take them out, and then do the Spleen Liver piece, and then call that good. And maybe four or five points altogether, whereas someone else, it might be 10 to 20. Kind of judging by both how novice they are at acupuncture, how they look, how strong’s their Qi—yeah.
Q: And is it different if they have like shoulder issues?
A: You mean like that was their chief complaint and their main reason for coming?
Q: Yeah.
A: Yeah. Different filters kind of move to the foreground. Whereas the person with menstrual problems, I’m not going to do a lot of manual muscle testing. Maybe at some point, I might want to find out what’s going on there, but I probably would skip that for the menstrual case. For the shoulder guy, yeah. That’s going to—I mean, I’ll do the tongue and pulse, and whatnot, and just kind of get a sense, “Jesus, his pulse is big and wiry. OK.” We know that moving things is going to be a more important factor than tonifying, whereas somebody who’s very kind of slight and tired, and their pulse is really weak, it’s like, “Oh, I think before I drill into the muscles that I’ve discovered need to be happening—I’ve don’t my manual muscle testing,” but I’ve done my pulse, and it’s like, “We need to give her a little Spleen 6, Stomach 36, or something,” either that I’ve found through Shu point testing or just in general. I need to brace her up a little before I start trying to attempt to move a lot of energy in her shoulder. Because if she’s already kind of this way, it won’t work out well.
Q: Yeah. So, you do your manual muscle testing, you get a sense of the TCM diagnosis, they’re laying down on the table, and the first thing that you do is…
A: Give them a big kiss. No.
Q: Would it be like you said earlier, like you would try to do a couple points to calm them down?
A: Mhm, or even before that, for a lot of cases, the very first thing I do with them is I pot your Shin-Min [?] in. Because I know that they’re kind of hyperreactive, wiry types. And it’s like, that, I know, will take off about 30% of that tendency. Pop those in real quick. Or Shin-Min with Sympathetic, if they’re real type-A and they’re always constantly in sympathetic mode. Pop those two in, and then like, “OK, now what?” Then, maybe I’ll do the Shu points. The Shu-point designated body points.
Q: Is that a good rule, in general, to kind of throw in Shin-Min to kind of calm them down first before you palpate the Shu points?
A: I don’t usually do it before I palpate. I usually do it as sort of the overture to the treatment. I sometimes think of treatments as being sort of a musical piece, like, “OK, here comes the overture, or here comes the first act.” OK, they’ve come off the ceiling; their fingernails are no longer stuck in the ceiling. Great. Now we will need them to arrive on the table. And we’ll do the Spleen 6 and whatever else. Now, they’re kind of fully present. Now, I can kind of take apart the knottier areas.
So, sometimes, it may not be actually three discreet sets of needles, but it may kind of progress in that fashion.
Q: How long are treatments?
A: For me?
Q: Yeah.
A: Usually an hour to an hour and a quarter. Between talking with them, getting them changed and getting them out the door.
Q: OK, so, I’m palpating, and I find the Shus, I test the points, and I don’t have the palpation. I can’t seem to find anything that seems to work.
A: Something that releases it?
Q: Yeah. Do you ever needle locally?
A: Yeah, you can, sure. Or let’s say they have pain at Bladder 43, and I find that Pericardium 6 releases it some. Will I flip them over if I’ve had them supine, and go locally? Of course. You bet. Especially if there’s a local problem. And then I may follow it up with some Gua Sha [?] or something. Yeah, definitely.
Q: Is it a light pressure, is it a strong pressure?
A: To the point that you’re testing?
Q: Yeah.
A: Pretty light. I mean—
Q: Do you ever find that it’s light, and then if you press harder, it releases, or does it tend to be pretty light?
A: I would say light to medium. I mean, basically, what you’re doing is you’re asking a question. And I think it may help a little bit if you’re actively asking the question in your mind, you know, intention. It’s like, “Hey, what do you think of this? How about this? How about that?” It’s almost like you’re asking the body. It’s like what I was doing with you earlier, like with the manual muscle testing. It’s like, “What does your body think of this? What do you think of that?” So, it’s this questioning mode. It’s asking the person, “What do you think of this? Is this important?” And it doesn’t need to be heavy pressure. I mean, you don’t want to just barely touch it. You want to make contact so enough so it’s like, “What do you think of this?”
But if you’re getting equivocal results, try changing the vector. Like pulling or pushing or lifting or—sometimes that’ll, like, Dr. Tran, in our doctorate program, he said that he always uses Kidney 7 towards 8. And I was like, “I’ve never heard of that.” And he said, “Oh, very important.” And it was like, hm. So, what I’ve noticed is sometimes, I’ll be looking for a kidney point, and I’ll kind of go over 7, and it was like, “Oh, there was something in the area,” and, “Did you try 7 toward 8?” and I’ll put it on 7 and pull toward anterior, and it’s like, “Oh, that’s it.” It releases with that vector. That’s the way you have to needle it.
Q: So, I palpate a Shu, find the tight spot. Do I decrease pressure, touch a point, and then push again? Or do you leave it on that tension and touch points? You know what I mean?
A: I strum the Shu point with each point.
Q: Strum it, and then stop strumming, test, and strum again? Like playing a guitar?
A: Yeah. Like, “What do you think of this point? How about this point? How about this point? Oh my god, I didn’t even have to strum. I could just feel my finger sink in.” But usually, there will be a little leveraging off my knuckles here, kind of going, “Ee-ee-ee-ee.” I mean, I could show you, if you want.
Q: No, I that makes sense. And I think you already explained it in that paper that you sent me.
A: There’ll be more.
Q: I’m just getting it down so that we can—so, you graduated school—where did go to school?
A: Well, it was right after the earth cooled. We had to get the dinosaurs out of the way to get to class.
Q: Because three had to have been time before Kiiko started teaching, right?
A: Oh, god yes.
Q: Because Kiiko wasn’t teaching in the beginning.
A: Oh, no, I’ve gone through many iterations of practice style, heavens.
Q: OK, so you were—how old were you when you started studying with Kiiko, or looking into Kiiko? How far [?] after practice?
A: Oh, maybe 12 to 15 years, somewhere in there.
Q: OK, and then you started learning about Kiiko’s method, and really liked testing unresponsive [?], and so, started to explore that.
A: But I never became a full Kiiko acolyte. But I liked her emphasis on, stuff should happen right now. We should be able to find out what’s going to work, and we should be able to find out right now what’s going to be the most effective treatment for you, based on palpation. And I found that I had a facility for palpating, whereas, you know, maybe some five element practitioner, “Oh my god, I can tell by the smell, it’s acrid, so that means you’ve got this constitutional situation.”
Q: Yeah. I tend to be hands-on, so I think that’s why I’ve gravitated towards that style. How do you develop that, or teach it, to people that aren’t hands-on? How do you develop the sensitivity, how do you—yeah, how do you develop the sensitivity?
A: Practice. But what I find is that most people who are magnetized to acupuncture are tactile. They’re kinesthetic, tactile people. They want to do stuff with their hands, they want to do it with people, to people, all of that. Or you get people in Chinese medicine who aren’t that way, they gravitate more towards Chinese herbs, which is much more of an intellectual exercise, it’s more contemplative, it’s less about touching people.
Q: Does the translation—because there’s some thoughts that the theory of acupuncture and the theory of herbs are kind of two separate things, they don’t necessarily—so, does the Shu points—does the diagnostics that come with that, does that roll into your herbal formulas?
A: It can. It’s more for my acupuncture, but it will inform it. You know, like let’s say the case that I was talking about, where the liver pulse is both wiry and deficient. It’s kind of a little of both. It’s like, “Well, what’s most important for me to do with this person?” Or, “Gee, OK, we need to do more moving, perhaps.” The symptoms could be either way. They have some signs of Liver Qi stagnation, but they also have some signs of blood deficiency. Well, let’s do both. With herbs, you could do both, but what do you want to emphasize? But I think that by in large, it informs my acupuncture much more than my herbal medicine.
Q: OK. And you leave your hand at the point?
A: While I’m testing with the other one.
Q: Yeah. And they tend to be both bilateral. Do you ever test both sides, or do you just stick with the one side that’s easiest?
A: I tend to just stay on the one side, and then I’ll swing around to the other side of the table. Could you do it? Yeah, you could, but I try to use good body mechanics, and when I start getting too reachy, my back—
Q: Again, I know this is all theoretical, and—so, my hand’s on Bladder 23, and I’m testing kidney points, and I’m testing bladder points, and I can’t seem to feel like it’s releasing on the left side of the body, the side that’s closest to me. Do you ever find that it releases on the opposite side? Or is it pretty much just if you check one side, you’re probably going—it’s going to release the same?
A: Well, what happens often with that situation is I’ll go, “I’m not getting any clear reading. Let’s go over to the other side.” Sometimes I’ll get a clearer reading on the other side, and once I find the relationship, I’ll go back, and it’s like, “Yeah, that was it,” but it’s almost like going at it with fresh eyes, going around to the other side.
Q: OK. So, that is a thing. If you do not find it, you can go check the other side.
A: The other thing is being open to other point locations. For instance, a lot of times the SI 15 area, like, it’s an SI point, maybe, yeah, but for instance [phone rings]. What was I talking about?
Q: Testing both sides, and then alternate point locations.
A: Oh, yeah. So like, Small Intestine 7. Small Intestine 7 can be anywhere from here to here. What you’re looking for is the spot that works. Or Liver 8 is kind of a big zone for me. And there’s a lot of points I use in different locations than the book, that’s where I was taught, or where a lot of people ein the olden days were taught. Like Lung 7 is here, not up here. So, sometimes it’s a different location that will garner it, or it’s an extra point. Like Bladder 19, I’ll check the gallbladder points, and I’ll go, “Did you check Dang-Mang Shue [ph.]? Ah, that’s it.” It’s a real gallbladder-oriented thing where you need to use Dang-Mang Shue. That’s the point that’s most important today.
Q: OK. Anything else I should know?
A: You start playing with it, and then you develop your own style, too. Like sometimes, for Bladder 13 or 42, it’s Lung 1. It’s not on the arm. It’s often the points out here are more active, generally. The Antique Points, as they used to sometimes be called.
Q: That actually is interesting.
A: The points from like the knee down and the elbow down. Those are influential points. They tend to be more influential than some of the body. But sometimes the body points are the most important one. Like Liver 13 or 14 or Lung 1. And sometimes it’s above the knee, like Gallbladder 31 is often a really good point.