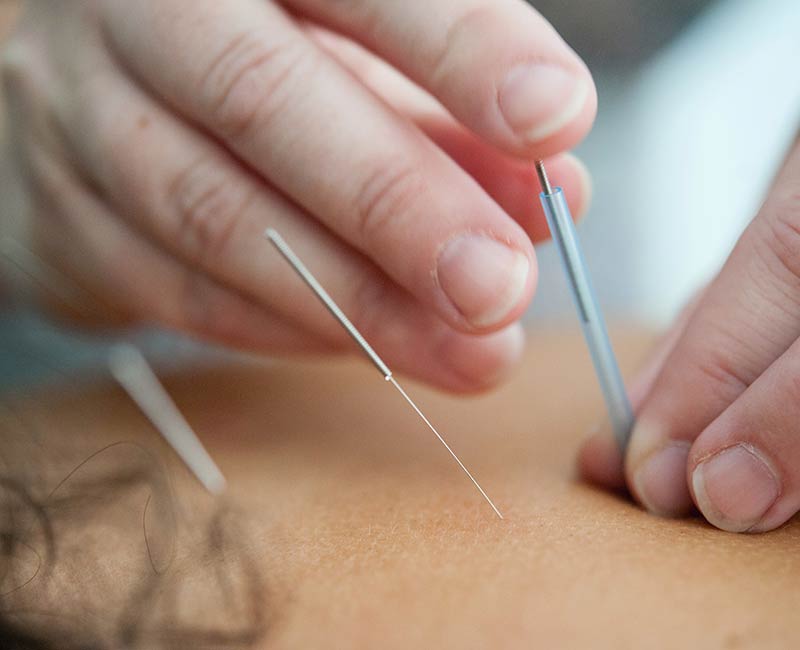
Back Shu Point Theory – Fast Facts
- The Shu points are often used diagnostically.
- Testing the Shu points allows you to get a sense of a patient’s response as it happens.
- There’s no specific needling technique—it’s about testing to figure out which technique works best in each situation.
- Shu Point diagnosis can impact your physical treatment/needling, as well as herbal treatments, but should mostly inform physical treatment.
Back Shu Points in Practice
- Affected Shu points can change throughout the day.
- Often, Shu point diagnosis can resemble “chronotherapy” because the time of day matters.
- The same point may be affected on multiple patients at the same time of day.
- Back Shu points tend to be (but aren’t always) paired.
- Occasionally a paired meridian, or you could have bleed-through to other points.
- Not always on the same channel.
- Back Shu points are easier to access while the patient is lying supine (face-up).
- You can get a more neutral reaction from the areas that aren’t involved.
- You get feedback from a patient’s face that lets you know how the treatment is going.
- The ANGLE of needling matters.
- A point will sometimes respond a little, then respond more as you change the direction of your needle angle.
- A point will sometimes not respond unless it is angled correctly.
- Testing the Shu points can help balance and relax the patient.
- Testing Shu points early in the appointment can promote better treatment later on.
- Think of having a conversation with each Shu point you’re testing. “Ask” the point, “How is this?” by your palpation and listen to its response.
What if you find multiple tight spots when you scan the Shu points?
- Combine what you feel with what the patient feels, but rely mostly one what YOU feel. Many people don’t live inside their bodies enough to realize they have tight points in multiple places.
- Often multiple points are related. Look for pairings and anglings that address both.
- The number of points you treat during a session depends on the individual—whether they’re new or experienced, etc.
- Take note of which areas were tight, and which points were affective, for reference at the next appointment.
Watching Your Patient
In the supine position, you can check in with your patient more easily. Things to check include verbal cues, as well as their color and expression.
Color
- Yellow – A slight yellow tinge is a good sign.
- Pink or red – Time to check in.
- Green or pale – Time to slow down!
Musculature/expression
- Facial expression or musculature seems to melt – patient is relaxed and will likely respond better to further treatments.
- Tightening up – Time to check in or slow down.
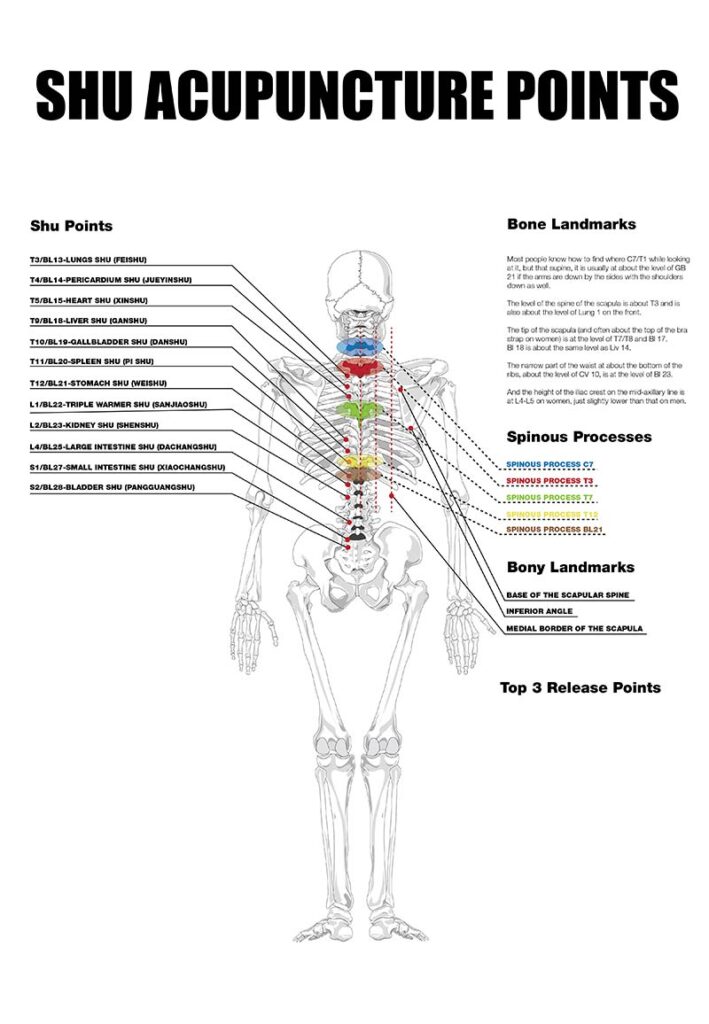
Treatment Flow Using the Shu Points
Check in with your patient if they’re new: what’s their experience with acupuncture? How do they feel about needles?
General Flow of Treatment:
- Assess the patient’s concerns—is it more musculoskeletal or more internal medical? Ask related questions based on their condition to gain information on which points to test.
- Test the tongue and pulse if it is the patient’s first appointment, or if they are a repeat patient with internal medical concerns.
- Start with patient in supine position to test the muscles, abdomen, and Shu points. You can then have them flip over when and if necessary.
- Palpate and test (light to medium pressure).
- Try changing from puling or pushing to lifting. Sometimes, the direction you push or pull a point makes all the difference.
- Strum the Shu point with each touch point.
- Start with the side closest to you. If nothing shows up, move to the other side of the table and test the same points on the other side.
- If no points apparently work, you may needle locally.
- You may needle the front mu points before addressing other areas to calm down patients who are Type-A, or in sympathetic mode. (Always make sure your patient is present and relaxed before treating tenser, knottier areas.)
- Place your needles and let the patient sit.
- Depending on the patient’s tolerance level and experience with acupuncture, come back and layer more or take out the needles and assess.
Your treatment flow may vary depending on the patient, their experience, and their needs:
Musculoskeletal concern (shoulder problem, etc.)
- Check tongue and pulse if it is a new patient. (If it’s a repeat patient with the same concern, you don’t need to do this each time.)
- Scan Shu points (helps to balance and relax the patient)
- Manual muscle testing takes primacy.
Internal medical concern (menstrual issues, etc.)
- TCM takes primacy – check tongue and pulse each appointment.
- Scan the Shu points (Spleen 10 is a good point for gynecology, Liver 13 is the move point for the Spleen.)
- Tension points will most likely be bilateral.
Treatment Examples
1. You’re at the insertion point at the levator scapula, and you notice it’s very tight. You put one finger on that point. You then put the fingers of your other hand on the motor point of the flexor carpi ulnaris, which is often very affective for this point. The levator scapula melts away immediately. From this, you know that the flexor carpi ulnaris will be the affective point for the levator scapula.
2. You check your patient’s pulse and notice that their liver pulse is a little empty, tight, and wiry. To decide whether to focus on tonifying or on moving, you test Liver 14 and notice it releases Bladder 18 completely, therefore making moving your focus area.
3. You’re scanning the patient, and notice that the medial scapula area is extremely tight. You palpate point 42, and the patient reacts with a strong, “Ow!” However, they never told you they had a should problem when they came in. You palpate some lung and pericardium points and feel the tension melt. (Remember to base treatment off of what YOU feel, as well as what the patient tells you!)
About the Author
Willard Sheppy is a writer and healthcare practitioner who seamlessly melds scientific knowledge with practical applications in engaging and authoritative articles. He holds a Bachelor of Science in Environmental Science from Oregon State University and a Master’s in Acupuncture and Oriental Medicine from the distinguished Oregon College of Oriental Medicine.
In his work, Willard skillfully combines his extensive educational background in scientific research with his practical experience as a healthcare practitioner. Willard balances his life with martial arts and cherished family adventures. As a father of three, he often leads his family on camping and hiking trips along the breathtaking Oregon coast.
Connect with Willard on LinkedIn at linkedin.com/in/valleyhealthclinic or learn more about his services at valleyhealthclinic.com. Embark on this journey towards holistic health with Willard!