What is Microcirculation?
Microcirculation is the circulation of the blood in the smallest blood vessels. It is the central location for nutrient exchange. Microcirculation is highly responsible for getting what your body needs to where it needs to go.
Functions and Responsibilities
Microcirculation plays a vital role in the transportation of:
- Nutrients
- Oxygen
- Hormones
- Waste Products
- Water
- Heat
- Respiratory Gases
–between the blood and body’s tissues and organs.
It can also play a role in the release of metabolic products.
And just like any busy street at rush hour, when microcirculation is disrupted in a traffic jam, it stops the nutrients from spreading to neighboring tissues.
A microcirculation traffic jam can make a person feel lethargic and weak without necessarily having anything noticeably wrong with them.
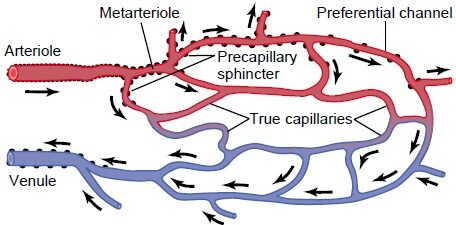
And at the base of this transportation highway is the capillary bed, an interwoven network of capillaries that bring nutrients to an organ and take waste products away.
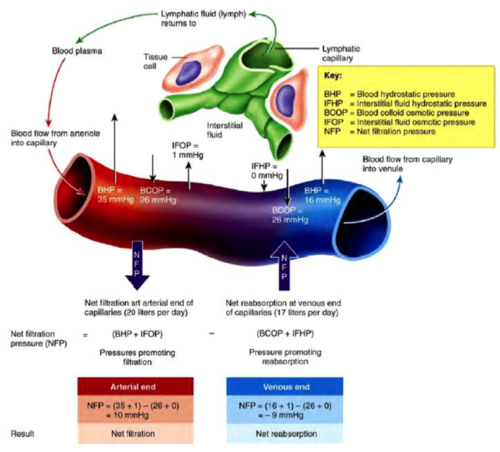
The capillary bed works with two main pressures. One that pushes things out of the vessel and one that pulls things into the vessels. Hydrostatic pressure from our heart pushes things out of the blood vessels and the osmotic pressure exerted by the proteins in our blood pulling things into the blood vessel . At the arterial end, closer to the heart there is more pressure from the heart so more things go out of the blood vessel, but on the venous end, further from the heart, the pressure from our heart decreases and there is more force pulling things into the blood vessel. Overall, across the entire circulatory system, there is more flow going out of the blood vessel and into the neighboring tissue. This excess is then picked up by the lymphatic vessels, cleaning out the excess and looking for pathogens.
What is Vasomotion?
Seemingly small in size but rather significant in function, Vasomotion, or Flowmotion Vasomotion, is an intricate, rhythmical contraction–relaxation mechanism that occurs in our capillary beds.
Vasomotion is the traffic lights of our circulatory roadways. It responds and adjusts perfectly to not only the local coming and going but to the system-wide flow.
If you have ever watched a heist movie where a nerdy computer hacker takes over the street lights system, you will have an idea of what vasomotion is doing. By adjusting the stop-and-go of traffic, the computer hacker controls the flow to help the thefts escape from the police. This is the basic idea of what vasomotion is doing, but rather than one heist taking place, there are many all over the city. Vasomotion helps control the flow of traffic in our body, so that it can operate more smoothly and efficiently.
What does Vasomotion do?
Vasomotion continuously adapts blood flow to meet the needs of the tissue nearest to it and the body system-wide.
This adjustment happens primarily in our arterioles, a small branch of an artery leading into capillaries, where our fluid and nutrient exchange is regulated between our vascular system and tissues.
When we think about arteries and veins, we often imagine them as passive tubes through which the heart pumps blood.
However, arteries are anything but passive. They actively pump, constrict, and dilate to help move blood through our arteries and veins. This contract and expansion process is called vasomotion.
This pumping mechanism of vasomotion optimizes the flow of blood and the exchange of energy.
This system is similar to how the lungs pump to move air. Although we have large passageways like the lung’s bronchial, there’s no oxygen exchange going on in there. Oxygen exchange happens at the smallest levels of the organ–the alveoli sacs.
Like our lungs, our large blood vessels can be considered dead space since oxygen exchange happens at the smallest level in our capillary beds.
Vasomotion is controlled by smooth muscle sphincters that dilate to allow blood flowing in and contract to increase blood flowing out. This pumping mechanism uses this cycle of motion to improve exchange efficiency.
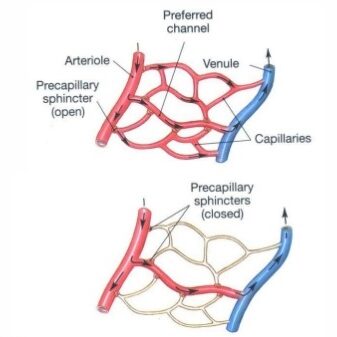
When contracted, capillary beds improve, clearing out excess fluid (swelling) and cellular debris because the net flow from tissue is out into the veins.
When they are open, they allow for improved exchange of nutrients and oxygen. If this opening and closing are not tightly regulated, then you can either have too much going out or too much coming into the tissue.

Vascular Autoregulation
If the vascular system were passive, there would be a linear relationship between blood pressure and blood flow. An increase in pressure would cause a rise in blood flow through an organ.
In fact many organs, including the brain and the kidney, are equipped with vessels that respond to a rise in blood pressure through vasoconstriction. Such vasoconstriction opposes the increase in blood flow that would otherwise cause pressure to go up in a totally passive vascular system.
So, with the opposing pressure, circulation stays stable. Autoregulation is achieved mainly by the arterioles.
This protects the capillary network from pressure variations, which would otherwise throw off the vessels’ equilibrium.
Vascular self-regulation has two functions
1) Ensures constant blood flow to an organ, even when arterial pressure changes.
For example, in the kidneys, the arterial resistance adapts automatically to falling blood pressure. But when systemic arterial pressure rises, kidney vasoconstriction occurs to maintain constant kidney blood flux.
2) Adjusts blood flow to the demand and need of organ activity.
For example, in active muscles, the circulation rate can be several times higher than the value of resting blood flow. To respond, blood vessels of the muscles open up to increase blood flow, and in areas that are less active, like the stomach, they will close down to decrease flow.
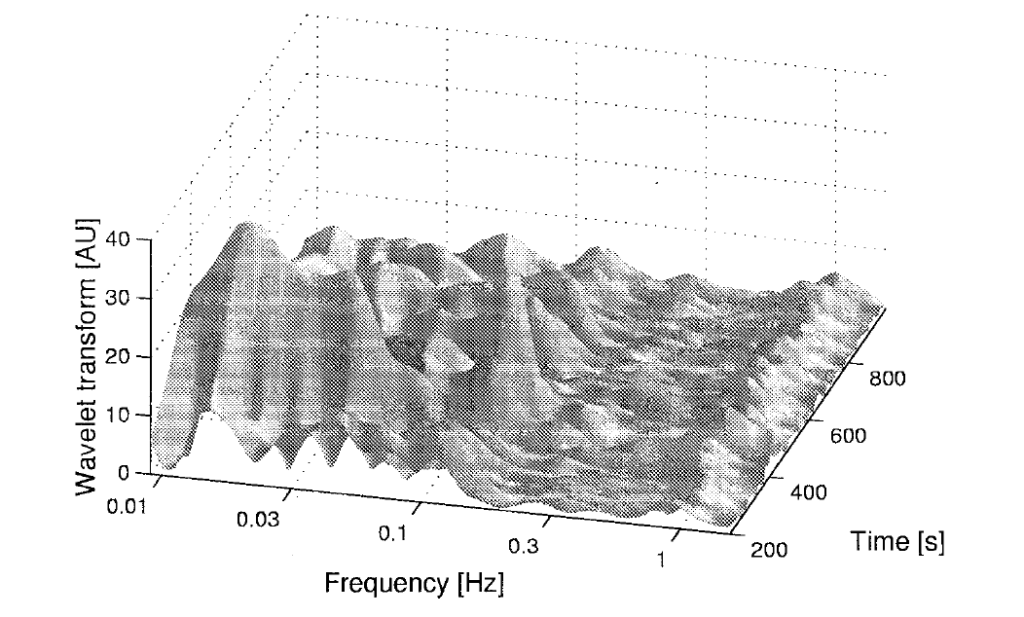
These adjustments of open and closing happen at different rates and frequencies. The fastest frequency of this is responding to our heart rate, closely followed by breathing respiration, and smooth muscle contractions.
I want to show you how to affect the vasomotion frequencies in your body. Later, you will learn how techniques affect each frequency and how they work together to balance the body. But first, let’s go over these frequencies real quick.
Cardiovascular Activity
0.97 Heart 1.66 – 0.625 second to cycle (1 sec).
Around 1 Hz, corresponding to cardiac activity.
The basic frequency near 1 Hz in the ECG signal, which dominates in the blood pressure, corresponds to the heart rate. At rest, it varies from 0.6 Hz in Athletes to 1.6 Hz in subjects with impaired cardiovascular systems.
The effect of the heart pumping is manifested in the vessels.
Respiratory Activity
0.27 Lungs 6.89-1.66 seconds to cycle (5 sec).
Around 0.2 Hz, corresponding to respiratory activity.
Modulation in this frequency interval corresponds closely to the respiratory.
The effect of breathing is manifested in the vessels
Smooth Muscle Activity
0.13 Smooth Muscles 6.89 to 18.86 seconds to cycle (15 sec).
Spontaneous activity recorded in microvascular smooth muscle cells was in the range .13hz
4–10 cycles per minute
The smooth muscles surrounding the blood vessels contract in response to an increase in intravascular pressure and relax in response to a decrease in pressure. This helps the blood flow to an organ stay constant.
This is called myogenic autoregulation. Myogenic is just a fancy term meaning coming from the muscles, and autoregulation implies that it is an automatic process that is not controlled by nerves.
Wavelet analysis has shown that the amplitude of myogenic oscillations is increased by exercise and decreased by local cooling.
Nervous System Activity
Autonomic Nervous System 18.86 to 47.61 seconds to cycle (30 sec).
Around 0.03 Hz, corresponding to neurogenic activity.
The autonomic nervous system can impact all the above systems: Heart, Lungs, Smooth Muscles
The autonomic nervous system innervates the heart, lungs, and blood vessels, except capillaries. The autonomic nervous system maintains the base level of contraction of the vessels. The nerves cause the release of substances that affect smooth muscles’ activities, leading to changes in the vessels’ radii and resistance.
That means that the nervous system takes part in vasoconstriction. A peak of around 0.03 Hz was observed in blood pressure, blood flow, and heart rate variable signals.
Nitric Oxide Endothelial Activity
Endothelial metabolic 47.61 to 105.26 seconds to cycle (1 min).
Around 0.01 Hz, corresponding to Nitric Oxide-related endothelial activity.
The blood supplies the cells with nutrients and removes their metabolism’s waste products while circulating the circuit of vessels. Substances related to metabolism, such as O2, CO2, NO, and lactic acid, directly affect the vascular musculature’s state of contraction. The control of the blood flow based on the concentrations of cellular metabolism is termed metabolic regulation.
It seems that the activity of endothelial cells mediates metabolic regulation of the blood flow by adjusting the concentrations of various substances. Nitric oxide (NO) is one of the most essential vasoactive substances.
Prostaglandin Endothelial Activity
Endothelial activity 105-200 seconds to cycle (2 mins).
Around 0.007 Hz, apparently corresponding to Nitric Oxide-independent (probably prostaglandin-dependent) endothelial activity.
This frequency was not identified in some of the earlier studies because the 20-minute recordings provided insufficient low-frequency resolution, and these oscillations were filtered out during data pre-processing.
However, a strong peak was later observed around 0.007 Hz ] and is clearly evident in the present work. This frequency was found to differ between healthy subjects and heart failure patients.
How Does Vasomotion Affect Us?
Knowing about vasomotion can be great for a medical student, someone learning or working in the health field, and someone looking to understand more about how their body works.
Let‘s take a closer and more realistic look at how vasomotion can affect our health in a day-to-day way:
When there are changes in the frequency of opening and closing of our capillary beds, these characteristics can lead to certain diseases. These indications were so strong that in severe cases, vasomotion improvement was actually considered a better indication of survival rate than the typical vital signs of heart rate, blood pressure, etc.
And on the flip side, a decrease in vasomotion increases the likelihood of death.
Disease Changes in Vasomotion
Vasomotion can actually change because of certain common diseases
For example, obesity and diabetes change vasomotion:
Obesity
The importance of a metabolic component has been supported by reducing all types of vasomotion in obese patients, regardless of diabetes status. The demonstration that sustained weight loss can fully normalize vasomotion in the skin.
Fibromyalgia
Apart from widespread pain, which is the main symptom of fibromyalgia, a great variety of functional changes occur in this disease’s presence.
Such changes include alterations in microcirculation, which may cause pain. There is a reduction in regional blood flow above “tender points” in fibromyalgia patients compared with healthy controls. Microcirculatory improved over the tender points in fibromyalgia patients after acupuncture therapy. This data suggests that acupuncture is a useful method to treat fibromyalgia patients as it can alleviate pain
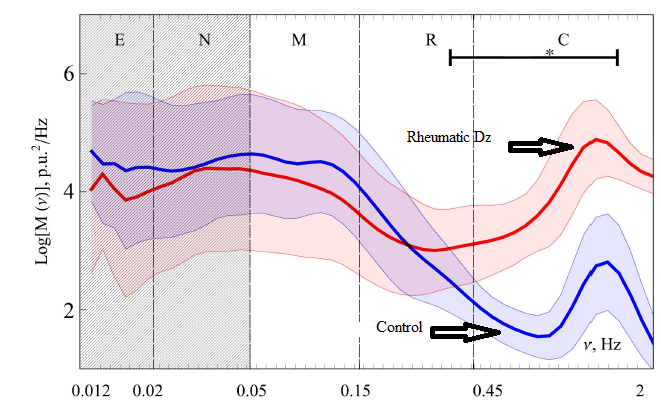
Rheumatoid Disease
Patients with Rheumatoid Disease had significantly higher-averaged blood saturation in base conditions in comparison to health people. Higher amplitudes of oscillations in the frequency range above 0.1 Hz (Cardiac Activity) were observed for patients with rheumatoid disease. This can be explained by the structural and functional changes in microcirculation occurring in the development of rheumatoid disease
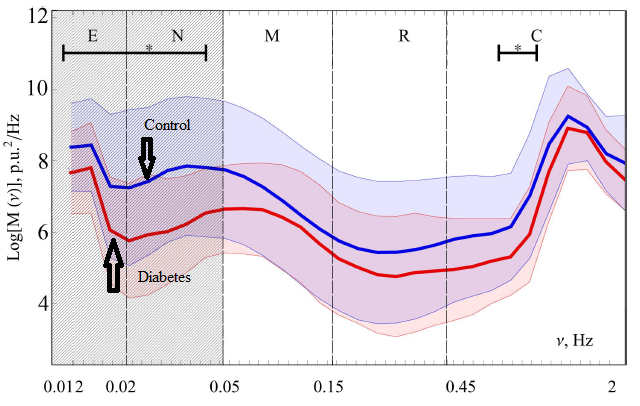
Diabetes
There is substantial evidence that diabetes, both in humans and in experimental animal models, is associated with an altered pattern and/or reduced prevalence of vasomotion.
For diabetes, the reduction of vasomotion is from a decrease in the frequency of the autonomic nervous system. The sympathetic innervation alteres vasomotion in diabetes is partly due to the associated neuropathy..Vasomotion affected by diabetes has a frequency of 0.012-0.045 Hz,), which is the frequency range associated with influence from the sympathetic nervous system and because the abnormality is predominantly seen in diabetic patients with neuropathy.
The effect of insulin on the endothelium is significant for the enhancement of capillary perfusion and glucose uptake in skeletal muscles. It has even been suggested that impaired vasomotion in type 2 diabetes may favor the development of high blood pressure.
Subjects with Diabetes M had impaired amplitude of blood flow oscillations in the frequency band 0.012-0.045 Hz, which corresponds to endothelial and neurogenic vascular tone regulating mechanisms.
Septic shock
Septic shock is characterized by profound hemodynamic alterations associated with organ dysfunction.
These hemodynamic alterations include some degree of hypovolemia (a decreased volume of circulating blood in the body) and a decrease in vascular tone, and myocardial depression. Even when systemic hemodynamic variables seem to have been corrected and are within therapeutic goals, signs of impaired tissue perfusion may persist.
Recently, alterations in microcirculatory blood flow have been identified in severe sepsis, and the severity of these alterations is associated with a poor outcome.
Microcirculation is so important even when all other vitals are normal. Alteration in microcirculation is a great indicator of mortality in septic patients.
You can have one capillary bed open right next to one that‘s closed. This would mean that some tissues would be getting oxygen right next to tissues that are without oxygen.
This decreased capillary density results in an increased diffusion distance for oxygen.
If microvascular blood flow is not congruent. You can have perfused capillaries in close vicinity to non-perfused capillaries. This leads to alterations in oxygen extraction and hypoxic zones even when total blood flow to the organ is preserved.
Heterogeneity or inconsistency in microvascular perfusion is a crucial aspect. Heterogeneous perfusion leads to more severe alterations in tissue oxygenation than homogeneously decreased perfusion does. Heterogeneity of perfusion is associated with heterogeneity in oxygenation but also has altered oxygen extraction capabilities. During episodes of hypoperfusion, the heterogeneity of microvascular perfusion further increases in sepsis instead of being minimized as in normal conditions.
These alterations play an important role in the development of organ dysfunction. They‘re not just an indication of the severity of sepsis.
Microvascular alterations can lead to cellular injury, and reversal of these alterations is often associated with improvement in lactate and mitochondrial function, suggesting that microvascular alterations directly impair tissue oxygenation.
In addition, several trials have demonstrated an association between the severity of microvascular dysfunction and the development of organ dysfunction and mortality.
What can we do to improve our microcirculation?
We need to do activities that regulate and improve or vasomotion frequencies. We need to bring into balance our Autonomic Nervous System which regulates our Heart and Lungs. We need to use gentle exercise and hydrotherapy to improve our smooth muscle frequency. Breathing and movement techniques that can balance nitric oxide and other vasodilating gasses in our body.
Below is a chart where I have provided preferences towards certain frequencies. Boxes that have three squares have a larger impact on that frequency than those with one.
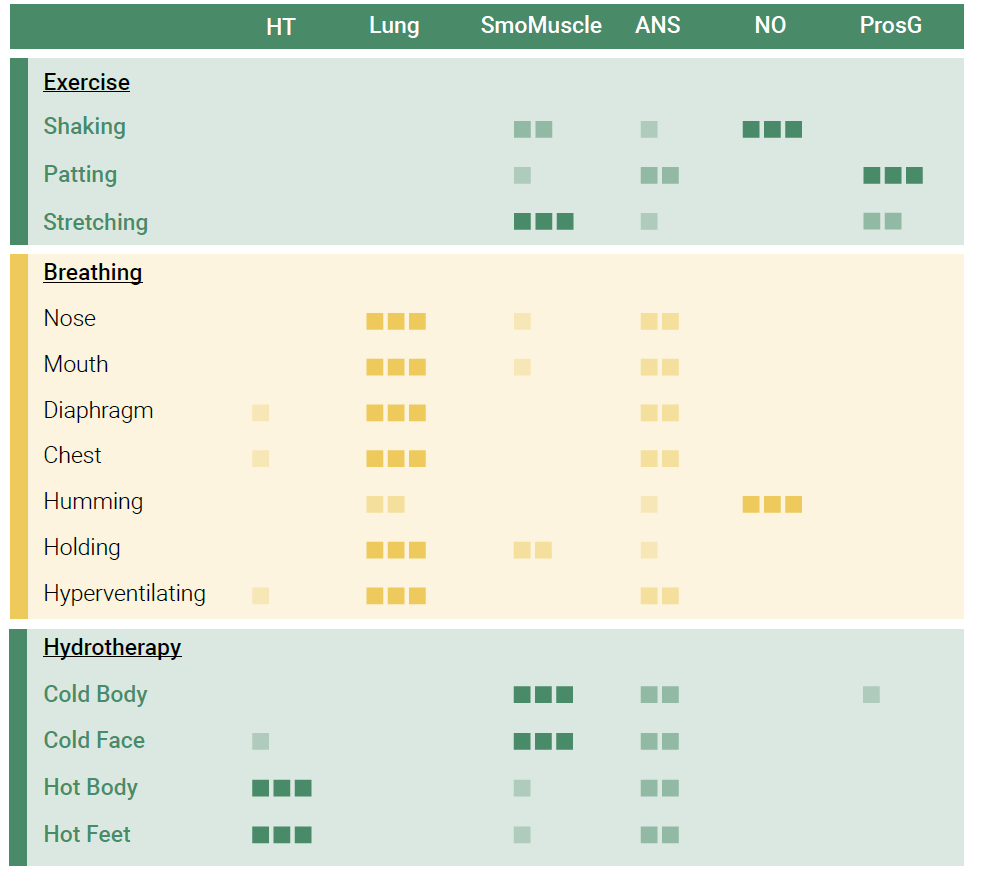
In the following article, we will examine movement and exercises to improve vasomotion. There is no direct one-to-one correlation, but preferences toward certain exercises and frequencies exist. For example, changing our breathing will affect our respiratory vasomotion frequency but also impact our autonomic nervous system frequency. We also know that hydrotherapy has an impact on our smooth muscle frequency.
About the Author
Willard Sheppy is a writer and healthcare practitioner who seamlessly melds scientific knowledge with practical applications in engaging and authoritative articles. He holds a Bachelor of Science in Environmental Science from Oregon State University and a Master’s in Acupuncture and Oriental Medicine from the distinguished Oregon College of Oriental Medicine.
In his work, Willard skillfully combines his extensive educational background in scientific research with his practical experience as a healthcare practitioner. Willard balances his life with martial arts and cherished family adventures. As a father of three, he often leads his family on camping and hiking trips along the breathtaking Oregon coast.
Connect with Willard on LinkedIn at linkedin.com/in/valleyhealthclinic or learn more about his services at valleyhealthclinic.com. Embark on this journey towards holistic health with Willard!