What Is Stretching?
Stretching is something that we all do. You’ll see dogs do it when they get out of bed. They’ll stretch, then yawn. You’ll see babies do it. It’s a natural process of being a human and animal.
Many people make the incorrect assumption that when muscles are tight, you need to stretch them, and by doing so, you will gain flexibility and muscles physically become stronger which is incorrect. Our muscles don’t really stretch. What we’re doing is we’re stretching our connective tissue and neurologically retraining our muscles.
If you feel that you are not flexible, it is not because your muscles are tight. It is because your brain is not allowing your muscles to move along to their full length. Your nervous system is inhibiting your muscles from changing their shape as a safety precaution. Flexibility is about gaining control over your muscles; it’s not about stretching them.
One of the aspects that Connective Tissue stretching is doing, is giving your nervous system a signal that you are fully in control, that you’re strong enough to protect yourself in that this position is not harming you.
Stretching
Stretching of any kind helps improve recovery and performance. Choosing the right type of stretch depends on two things:
- The type of activity you are doing
- Whatever gives you the best results
A good rule of thumb is you should enjoy stretching. You should not hurt while doing it and you should feel better, not worse afterward.
There are two major components. There’s the muscle component and there’s a connective tissue component. Let’s talk about the muscle.
Connective Tissue
The connective tissue is your tendons, ligaments, and fascia. Ligaments are what connect bone to bone and your tendons are what connect your muscles to your bones. We don’t want to stretch ligaments and Tendons. They are meant to hold your things together.
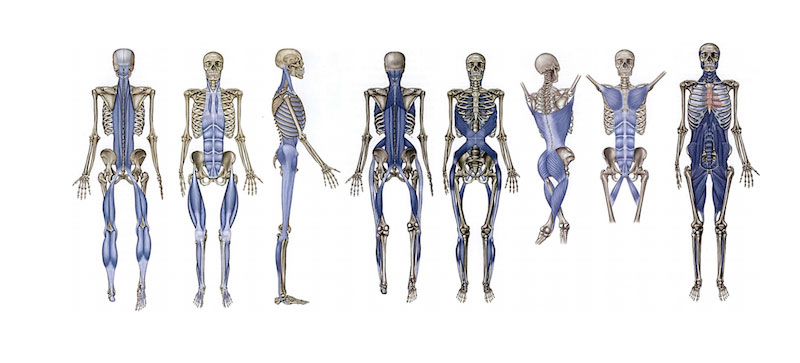
Outside of ligaments and tendons, we have fascia, a connective tissue that surrounds every fiber of your muscle. Not only around the muscle but also inside the muscle. Every single little muscle fiber has a little mini envelope of connective tissue around it. The whole muscle is wrapped in this multidimensional tube of connective tissue. The connective tissue doesn’t stop there, it goes between each muscle. This connection transmits the force from one muscle to the next.
We used to think the force that a muscle exerts, presses on the tendon and then presses on the bone. That’s no the whole picture a large component of the force that a muscle exerts, goes laterally to the connective tissue and around it, and then to the muscles beside it. Connective tissue distributes the force throughout the limb.
Connective tissue doesn’t just stop at the musculus, it surrounds every single organ in the body. This is what we call a matrix of connective tissue. It is the scaffold that gives our body shape. Connective tissue is the common denominator throughout the entire body. Fascia connective tissue literally connects us. It is what holds you together and provides your shape and posture. It is a state of structural and functional continuity between all of the body’s hard and soft tissues, Without fascia, our muscles would be like a jelly substance without much form at all.
This structure it provides is not passive. Fascial tissue contains contractile cells that influence musculoskeletal dynamics. Fascia is one of our most important perceptual tissues The fascia contains sensitive nerves that convey proprioception (joint position sense) fascial tissue is one of our richest sensory organs. A myriad of tiny unmyelinated ‘free’ nerve endings are found almost everywhere in fascial tissues, but particularly in bone and visceral connective tissues.
Connective tissue is composed of a base substance and two kinds of protein-based fiber. The two types of fiber are:
- Collagenous connective tissue (consists mostly of collagen and provides tensile strength)
- Elastic connective tissue (consists mostly of elastin and provides elasticity)
The base substance is called mucopolysaccharide and acts as both a lubricant (allowing the fibers to easily slide over one another), and as a glue (holding the fibers of the tissue together into bundles). The more elastic connective tissue there is around a joint, the greater the range of motion in that joint.
Fascia, when healthy, forms a gliding interface with underlying muscle allowing free excursion of the muscle under the relatively immobile skin. When we’re stretching the connective tissue, we’re actually stretching the more elastic quality fibers.
Connective tissue is also responsive to heat. That’s why when you do a warm-up, you increase your body’s temperature, or when you take a hot shower, you feel more flexible as this tissue is more fluid. Just like every other tissue in your body, your fascia is made of water. It works better, moves better, and feels better when it’s wet. So, drink more water! We’re not just stretching muscle but stretching this connective tissue that flows throughout the body that goes into our organs.
Why It’s Important To Stretch Our Connective Tissue
When you stretch connective tissue it stimulates anti-inflammatory agents in the body. So stretching can decrease inflammation, specifically when you’re stretching connective tissue. One of the benefits, when we think about yoga and tai chi as being helpful with arthritis and other inflammation, is that we are stretching this connective tissue.
Acute inflammation is accompanied from its outset by the release of specialized pro-resolving mediators (SPMs), including resolvins (Resolvins are specialized pro-resolving mediators derived from omega-3 fatty acids), that orchestrate the resolution of local inflammation.
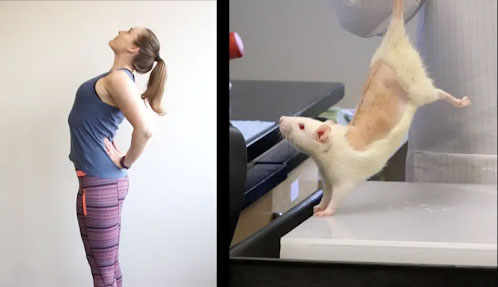
In rats with subcutaneous inflammation of the back, carrageenan was induced. Stretching for 10 minutes twice daily reduced inflammation and improved pain, two weeks after carrageenan injection.
Furthermore, subcutaneous resolving injection mimicked the effect of stretching. In ex vivo experiments, stretching of connective tissue reduced the migration of neutrophils and increased tissue RvD1 concentration. These results demonstrate a direct mechanical impact of stretching on inflammation-regulation mechanisms within connective tissue.
In a recent ultrasound study, human subjects with chronic low back pain had altered connective tissue structure compared to human subjects without low back pain, suggesting the presence of inflammation and/or fibrosis in the low back pain subjects. Mechanical input in the form of static tissue stretch has been shown in vitro and in vivo to have anti-inflammatory and anti-fibrotic effects.
Showed that gentle daily stretching for 10 minutes can reduce local connective tissue inflammation and fibrosis. Because mechanical factors within the stroma can influence the tumor microenvironment, they suggest a link between immune exhaustion, inflammation resolution and tumor growth. Stretching is a gentle, non-pharmacological intervention that could become an important component of cancer treatment and prevention.
What Happens When You Stretch
The stretching of a muscle fiber begins with the sarcomere, the basic unit of contraction in the muscle fiber. As the sarcomere contracts, the area of overlap between the thick and thin myofilaments increases. As it stretches, this area of overlap decreases, allowing the muscle fiber to elongate. Once the muscle fiber is at its maximum resting length (all the sarcomeres are fully stretched), additional stretching places force on the surrounding connective tissue. As the tension increases, the collagen fibers in the connective tissue align themselves along the same line of force as the tension. Hence when you stretch, the muscle fiber is pulled out to its full length sarcomere by sarcomere, and then the connective tissue takes up the remaining slack. When this occurs, it helps to realign any disorganized fibers in the direction of the tension. This realignment is what helps to rehabilitate scarred tissue back to health.
When a muscle is stretched, some of its fibers lengthen, but other fibers may remain at rest. The current length of the entire muscle depends upon the number of stretched fibers (similar to the way that the total strength of a contracting muscle depends on the number of recruited fibers contracting). The more fibers that are stretched, the greater the length developed by the stretched muscle.
Proprioceptors
The nerve endings that relay all the information about the musculoskeletal system to the central nervous system are called proprioceptors. Proprioceptors (also called mechanoreceptors) are the source of all proprioception: the perception of one’s own body position and movement. The proprioceptors detect any changes in physical displacement (movement or position) and any changes in tension, or force, within the body.
The fascia is highly innervated this the proprioceptive nerves. Especially the thoracolumbar fascia. They are responsible for sending information about joint position and movement. In chronic pain patients, proprioception is impaired and studies indicate that connective tissue structures in painful body parts exhibit pathological changes. Fascia should therefore be considered a cause of pain and proprioceptive deficits and treatment should be applied accordingly.”
Fascia is usually seen as having a passive role, transmitting mechanical tension which is generated by muscle activity or external forces. However, there is some evidence to suggest that fascia may be able to actively contract in a smooth muscle-like manner and consequently influence musculoskeletal dynamics. General support for this hypothesis came with the discovery of contractile cells in fascia, from theoretical reflections on the biological advantages of such a capacity, and from the existence of pathological fascial contractures.
How Connective Tissue Affects Flexibility
The resistance to lengthening that is offered by a muscle is dependent upon its connective tissues: When the muscle elongates, the surrounding connective tissues become more taut. Also, inactivity of certain muscles or joints can cause chemical changes in connective tissue which restrict flexibility. According to M. Alter, each type of tissue plays a certain role in joint stiffness: “The joint capsule (i.e., the saclike structure that encloses the ends of bones) and ligaments are the most important factors, accounting for 47 percent of the stiffness, followed by the muscle’s fascia (41 percent), the tendons (10 percent), and skin (2 percent)”.
M. Alter goes on to say that efforts to increase flexibility should be directed at the muscle’s fascia, however. This is because it has the most elastic tissue and because ligaments and tendons (since they have less elastic tissue) are not intended to be stretched very much at all. Overstretching them may weaken the joint’s integrity and cause destabilization (which increases the risk of injury).
When connective tissue is overused, the tissue becomes fatigued and may tear, which also limits flexibility. When connective tissue is unused or underused, it provides significant resistance and limits flexibility. The elastin begins to fray and loses some of its elasticity, and the collagen increases in stiffness and in density. Aging has some of the same effects on the connective tissue that lack of use has.
How Aging Affects Flexibility
With appropriate training, flexibility can, and should, be developed at all ages. This does not imply, however, that flexibility can be developed at the same rate by everyone. In general, the older you are, the longer it will take to develop the desired level of flexibility. Hopefully, you’ll be more patient if you’re older.
According to M. Alter, the main reason we become less flexible as we get older is a result of certain changes that take place in our connective tissues. As we age, our bodies gradually dehydrate to some extent. It is believed that “stretching stimulates the production or retention of lubricants between the connective tissue fibers, thus preventing the formation of adhesions”. Hence, exercise can delay some of the loss of flexibility that occurs due to the aging process.
M. Alter further states that some of the physical changes attributed to aging are the following:
- An increased amount of calcium deposits, adhesions, and cross-links in the body
- An increase in the level of fragmentation and dehydration
- Changes in the chemical structure of the tissues.
- Loss of suppleness due to the replacement of muscle fibers with fatty, collagenous fibers.
This does not mean that you should give up trying to achieve flexibility if you are old or inflexible. It just means that you need to work harder, and more carefully, for a longer period of time when attempting to increase flexibility. Increases in the ability of muscle tissues and connective tissues to elongate (stretch) can be achieved at any age.
Connective Tissue Stretching
There’s a different way to stretch when we focus on connective tissue versus when we focus on muscles. When you think about stretching a muscle you can very much isolate that muscle. If you want to do a hamstring stretch, you can isolate just a hamstring. When you’re focusing on muscles, it’s actually better to isolate a very specific muscle. When you think about stretching connective tissue, we want a large multi-complex movement that pulls on this connective tissue from many joints located at a distance from each other. We need to realize that although it feels like we are stretching, we are not really doing that.
It takes a lot of force or longer durations to permanently change fascia. Fascia nevertheless is densely innervated by proprioceptors/ mechanoreceptors which are responsive to manual pressure and stretching. Stimulation of these sensory receptors has been shown to lead to a lowering of sympathetic tonus as well as a change in local tissue viscosity. Additionally, smooth muscle cells have been discovered in the fascia, which seems to be involved in active fascial contractility. Fascia and the autonomic nervous system are intimately connected. A change in attitude in myofascial stretching needs to change from a mechanical perspective toward the inclusion of the self-regulatory dynamics of the nervous system.
Every person knows the experience of finding a tight spot in their body, massaging it, and feeling it “release” or “relax”. It seems natural to assume that you physically broke down a knot but this is not actually true.
Fascia collagen fibers are literally as strong as steel. To actually “break them up” would require so much force application that one’s body would sustain serious injury—this is not something that is achieved by a massage therapist’s hands or by simple stretching.
Although you may feel a tight spot in your body and change its texture after it is rolled, massaged, or stretched, this change was not the architecture of the fascia changing. When fascia changes its architecture, it does so slowly and over a long period of time—collagen takes about three years in order to completely change and remodel. Any instantaneous changes in tissue quality that you experience of stretching are not the “breaking down” of adhesions, knots, or scar tissue—they are instead changes in tissue tone that are mediated by the nervous system.
Once we wrap our minds around that connective tissue, stretching primarily works through neurological communication instead of physically breaking down adhesions, knots, and scar tissue. We need to realize the importance of being calm and gentle.
Connective tissue stretching involves stretches that utilize multiple joints and muscles. It is not isolating but encompasses the full body. It uses breath control and mental meditation to regulate the nervous system. The simplest example of this would be the sensation of a giant yawn and stretch in the morning.
When you yawn and stretch in the morning there is a breathing and a full body component. As your breath-in you contract and lean back, stretching your quads and your stomach. As you continue to breath-in and fill your upper chest your arms reach out and your mouth opens up engaging your face.
There is a full-body contraction, stretch, hold, and then the release as you breathe out. It stimulates and relaxes the nervous system. You feel this stretch everywhere and engage every part of your body and feel calm and refreshed afterward.
Head, Fingers, Toes
Connective tissue stretching uses the farthest ends of your connective tissue (head, fingers, and toes) to create different angles of tension throughout the body. There is an active component of pushing out with your hands or your feet to expand the body. Imagine pulling on the corners of a bed sheet to get rid of the wrinkles. You focus on your extremities, hand position, toe position, and head and eye position to pull and stretch.
Breathing with Connective Tissue Stretching
Proper breathing control is important for any successful stretch but particularly if you want to focus on the connective tissue. Proper breathing helps to relax the body, increases blood flow throughout the body, and helps to mechanically move and massage the organs. As you breathe in, the diaphragm pushes down on the internal organs and their associated blood vessels, squeezing the blood out of them. As you exhale, the abdomen, its organs and muscles, and their blood vessels flood with new blood. This rhythmic contraction and expansion of the abdominal blood vessels are partially responsible for the circulation of blood in the body. Also, the rhythmic pumping action helps to remove waste products from the muscles in the torso. This pumping action is referred to as the respiratory pump. The respiratory pump is important during stretching because increased blood flow to the stretched muscles improves their elasticity, and increases the rate at which lactic acid is purged from them.
The belly talks to the brain. Mechanoreceptors have been found abundantly in visceral ligaments as well as in the Dura mater of the spinal cord and cranium. It seems quite plausible that most of the effects of visceral or craniosacral osteopathy could be sufficiently explained by a simulation of mechanoreceptors with resulting profound autonomic changes. Recent discoveries concerning the richness of the enteric nervous system have taught us that our ‘belly brain’ contains more than 100 million neurons and works largely independent of the cortical brain. It is interesting to note that the very small connection between these two brains of a few thousand neurons consists of nine times as many neurons involved in processes in which the lower brain tells the upper one what to do, compared with the number of neurons involved in the top-down direction. Many of the sensory neurons of the enteric brain are mechanoreceptors, which – if activated – trigger among other responses, important neuroendocrine changes. These include a change in the production of serotonin – an important cortical neurotransmitter 90% of which is created in the belly – as well as other neuropeptides, such as histamine (which increases inflammatory processes).
Your breathing and your trunk are the links between your arms to your legs. It can be the difference between an isolation stretch and a full-body stretch.
Breathing in expanding the chest or diaphragm or both to engage the stretch. When you breathe into the chest you increase the stretch in your arms and neck. When you breathe into and expand the lower abdomen you can increase the stretch into your back and legs. Utilizing both techniques to create as much tension in the motion. Using the exhale to release that tension and create space for more movement. Even increasing the intensity of the stretch on the exhaling. Breathing in build tension, Breathing out relaxes the muscles and allows for more movement.
Example
An example of doing a static stretch and incorporating connective tissue techniques would be a traditional standing forward bend. This can stretch your calves and hamstrings. As you incorporate the breath and breathe-in, you will notice your lower abdomen expand and it will stretch your back. Then from your back, as you breathe into your chest you can tuck to your chin and stretch your neck creating a line of tension from your toes to the top of your head.
Use the breath to support movements that are complex or threaten the spine. Breathing in to create abdominal pressure to support the spine as you move until you are safe then exhale.
As you breathe deeply and steadily, you may notice an ebb and flow of you stretching that mirrors the tide of your breath. As you inhale, your muscles tighten slightly, reducing the stretch. As you exhale, slowly and completely, your abdomen moves back toward your spine, the muscles in your lower back seem to grow longer, and you can drop your chest toward your thighs.
It’s obvious that exhalation deflates the lungs and lifts your diaphragm into the chest, thereby creating space in the abdominal cavity and making it easier to bend the lumbar spine forward. (Inhalation does the opposite, filling the abdominal cavity like an inflating balloon, making it difficult to fold your spine forward completely.) But you may not realize that exhalation also actually relaxes the muscles of your back and tilts your pelvis forward.
How to Stretch
Warming Up
Stretching is not warming up! It is, however, a very important part of warming up. Warming up is quite literally the process of “warming up” (i.e., raising your core body temperature). Warm-up combined with stretching increases the range of motion greater than stretching alone. A proper warm-up should raise your body temperature by one or two degrees Celsius (1.4 to 2.8 degrees Fahrenheit) and is divided into three phases:
- General warm-up
- Stretching
- Sport-specific activity
General Warm-Up
The general warm-up is divided into two parts: instead of hitting the treadmill or grabbing the weights, try using shaking and patting to safely and gently raise your body temperature.
The best example of a vibration-type exercise is the shaking and patting you see top athletes do before a race or competition. Shaking out, and patting down, a muscle group or part of your body gets it engaged in much the same way as more strenuous exercise. Vibration and patting create a mechanical force that stimulates endothelial cells to release Nitric Oxide which increases blood circulation.
Start by shaking your hand and feet with small gentle movements. Then incorporate your knees and elbows then move your hips and shoulders and the last twist your spine side to side. Afterward, raise up onto your toes and drop to your heels.
Then you want to pat your skin and connective tissue. Startup your body feet to head and down your back. There should be no pain, just your hands and skin should get slightly pink.
These two activities should be performed in the order specified:
- Warming up body
- Joint rotations
Joint Rotations
The general warm-up should begin with joint-rotations, starting either from your toes and working your way up.. This facilitates joint motion by lubricating the entire joint with synovial fluid. Such lubrication permits your joints to function more easily when called upon to participate in your athletic activity. You should perform slow circular movements, both clockwise and counter-clockwise, until the joint seems to move smoothly. You should rotate the following (in the order given, or in the reverse order):
- Fingers, Toes
- Wrists, Ankles
- Elbows, Knees
- Shoulders, Hips
- Neck, Trunk/waist
Warm-Up Stretching
The stretching phase of your warm-up should consist of two parts:
- Connective Tissue stretching
- Dynamic stretching
It is important that Connective Tissue stretches be performed before any dynamic stretches in your warm-up. Dynamic stretching can often result in overstretching, which damages the muscles. Performing static stretches first will help reduce this risk of injury and mitigate any performance decrease.
About the Author
Willard Sheppy is a writer and healthcare practitioner who seamlessly melds scientific knowledge with practical applications in engaging and authoritative articles. He holds a Bachelor of Science in Environmental Science from Oregon State University and a Master’s in Acupuncture and Oriental Medicine from the distinguished Oregon College of Oriental Medicine.
In his work, Willard skillfully combines his extensive educational background in scientific research with his practical experience as a healthcare practitioner. Willard balances his life with martial arts and cherished family adventures. As a father of three, he often leads his family on camping and hiking trips along the breathtaking Oregon coast.
Connect with Willard on LinkedIn at linkedin.com/in/valleyhealthclinic or learn more about his services at valleyhealthclinic.com. Embark on this journey towards holistic health with Willard!